Laurie's Blogs.

Dec 2020
Professional practice is about the stuff between the ears…
A culmination of multiple different things led to this post and I didn’t really know what to call it. Essentially, what I want to talk about is clinical reasoning, but that’s not a captivating title!!! So instead, “Stuff between the ears” has a better ring to it! (Ha ha!)

Okay, so things that led to this blog.
1. A regular patient of mine has a strange sudden onset neurological episode without history of any trauma. They went to their primary care vet who did x-rays of the dogs back and commented that they didn’t see any issues, prescribed a non-steroidal and advised a wait and see approach or referral to the neurologist. The client brought the dog to me (as her regular therapist) and I found the dog to have full body ataxia, which, as the owner showed me, worsened when the dog looked up and to the left. Now, I’m guessing that most of you see the trouble – no neck x-rays were taken despite the ataxia being x4 limbs. Essentially, my clinical reasoning skills led me to assessing the neck which led me to finding pain with doing a stress test of the Alar ligaments. Fast forward: Note sent to vet. Treated with high doses of laser, PEMF, and home active ROM (small amplitude cookie exercises). Dog has improved to almost normal. Owners are happy. Vet has told owners how amazed she was that I had found this. And why did I find this? Clinical reasoning.
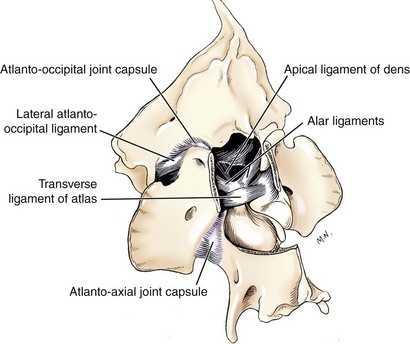
Picture from: https://veteriankey.com/surgery-of-the-cervical-spine/
2. I saw a FB post about a case where the rehab DVM was ‘beating herself up’ for a case that turned out to be neoplastic in origin. I never did get around to responding on that post, but I meant to post about learning from the case (see my point number 3 below) and using that for future cases when the presentation doesn’t add up to what you would expect to see for a certain diagnosis (or presumed diagnosis).
In this case, I was reminded up was a Newfoundland Dog that I saw as part of her maintenance check-ups / treatments. The owner was about to leave for a 10-day trip out of town but had noted that the dog was a little lethargic lately. Clinically speaking, lethargy isn’t a typical finding in musculoskeletal cases. So, I had mentioned that she should set an appointment with her vet about that when she returned. However, on my exam, I found a huge axillary lymph node (as in the size of a hockey puck)! I pointed it out to the owner and told her to see her vet immediately, that this shouldn’t wait until she was back from her trip. I sent a note to the vet, and let the owner know that this was concerning enough to NOT postpone a consult. Fast forward: Her vet got the dog in that day and found the dog had pyometra and was put on antibiotics immediately and a spay was done shortly thereafter. The owner said that the vet was amazed – “Laurie found this (as in the lymph node)? Laurie told you to come right away?” And why did I find this and respond the way I did? Clinical reasoning.
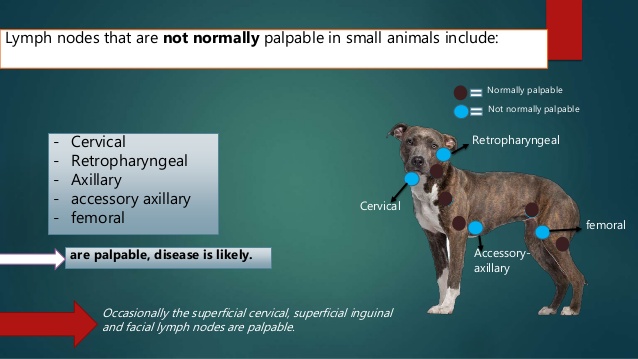
Picture from: https://www.slideshare.net/GansbaaiSA/examination-of-superficial-lymph-nodes-in-dogs-and-cat
3. In the same week, I saw another post where a vet physiotherapist was asking about a dog with severe atrophy of the scapular muscles and lameness that came on after a prolonged period of ‘rest’. In this case, I responded raising the suspicion of a nerve sheath / peripheral nerve tumour.
This case reminded a dog that I had treated years ago. She had a front leg lameness. Her vet had x-rayed the dog’s neck and leg and authorized a rehab consult. I found mild supraspinatus tenderness. Treated that but the dog was still lame. Found ‘maybe’ mild biceps tenderness and ‘maybe’ some medial shoulder hypermobility. Treated that, but no change in lameness. Treated the neck and cranial thoracic spine & ribs, just presumptively, but still no lameness improvement to be had. Unfortunately, the owner moved across the country, but we facilitated a transfer of records to a practitioner near her (a Rehab Vet Tech) who eventually facilitated a referral to a neurologist. They found a nerve sheath tumour. Kudos to the tech! And for me, this was my first nerve sheath tumour case and I have never forgotten the presentation, the lack of response to treatment, and the dramatic atrophy of the scapular muscles despite lack of a structure to pinpoint as the cause. I learned from that case. I never forget that case. I vowed I would never miss one of these again. And since then I have counselled dozens of other practitioners (of all disciplines) on how to recognize nerve / nerve sheath tumours. How did I get to this point? Reflective practice as part of my clinical reasoning.
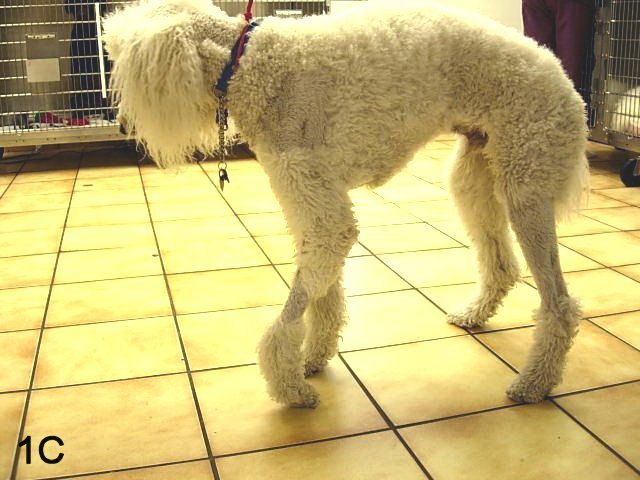
Picture from: https://brewerneurovet.com/peripheral-nerve-sheath-tumors/
4. There have been discussions on various forums, in direct messaging, and in my dealings with various veterinary boards on concerns regarding concerns over non-vets treating animals that seem to start with “What if…” Follow that with various clinical scenarios. I’ve been wracking my head to come up with a way to express how as a physiotherapist, when I approach a patient, it is not just with a bag of tools and tricks, but it also includes my clinical reasoning skills. Fundamentally, they are the underpinning of the profession of physical therapy.
Communicating clinical reasoning as a skill set is a tough one. Then I remembered a form that we used for presenting a case study as part of my Master's Degree in Animal Physiotherapy. I have turned it into a document, and it can be downloaded from here:
https://www.fourleg.com/media/Clinical%20Reasoning.pdf
I was going to post it in point form… but it would lose context. All in all, this is how I think when I approach a patient, with each and every appointment. This is how I was taught to think as a Physiotherapist, and this form was created by Physiotherapists to help us as students in the animal physiotherapy program to remind us continue to Think Like Physios even when facing an animal patient compared to a human patient. I love this form and I’d encourage anyone in animal rehab practice to try using it as a way to enhance your clinical practice.
On that note, I wish you a wonderful week ahead and Happy Clinical Reasoning!!!

